FRIDAY, 7 JULY 2017
Neonatal diabetes is a myth. At least that was what Frances Ashcroft was told in 1997 on her quest to find newborns with the condition. Yet her persistence and determination to find the cause and cure of this unique condition was unfailing. Not only did she discover the disease, she also pioneered a better treatment that would prove invaluable to patients. One young girl burst into tears telling Ashcroft, “I can wear a dress again!” because she no longer needed to wear a belt for her insulin pump, avoiding the dreaded daily insulin injection. Not only had Ashcroft replaced needles with an oral drug, she had allowed these children, and their parents, to lead a more normal life.It was previously thought that there were only two types of diabetes: a type of diabetes caused by several genetic factors, and a type of diabetes caused by environmental factors, such as diet. This assumption led to the misdiagnosis of newborns who suffered from a third type of diabetes caused by a mutation in a single gene. This was often accompanied by delayed development and neurological disorders. If Ashcroft had not dug deeper, the simple treatment for these conditions may have remained buried.
4.5 million people in the UK currently suffer from diabetes. Diabetes occurs when there is insufficient insulin to maintain blood glucose levels, which can lead to numerous health problems. Insulin, discovered in 1922, is the hormone released by the pancreas following a meal, which keeps blood glucose levels stable. There are two common types of diabetes called Type 1 and Type 2 diabetes. In Type 1 diabetes the immune system attacks and destroys the beta cells of the pancreas, which are responsible for the production of insulin. In Type 2 diabetes, the pancreas fails to produce enough insulin or the body becomes insensitive to it.
 Professor Dame Frances Ashcroft
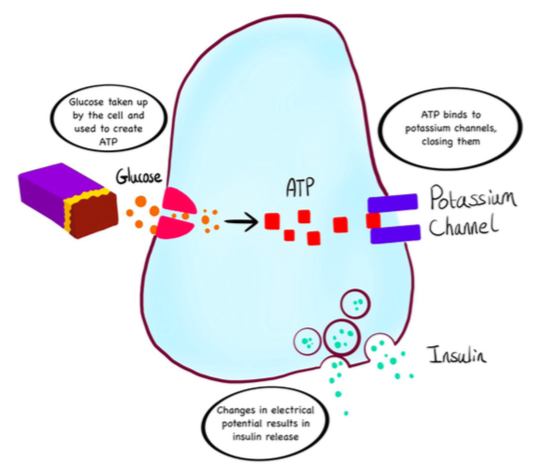
Professor Dame Frances AshcroftAfter completing her degree in Natural Sciences and her PhD at Cambridge, Ashcroft joined the University of Oxford as a research fellow in 1984. She wanted to use this position to research something of medical relevance, unlike her previous work on the muscles of stick insects. She decided to explore why increased blood glucose levels cause the pancreas to release insulin. In her initial experiments on rats, she found that glucose closes a pore in the surface of specialised cells in the pancreas. This pore, called a potassium channel, normally allows potassium ions to flow out of the cell, closing when insulin is released. In 1985, Ashcroft discovered the role of the pore. Glucose is taken up by the cell and used to produce a molecule called ATP. ATP binds to the potassium channel. This leads to some electrical activity in the beta cells and insulin release.
A drug called Sulphonylureas is able to induce low glucose levels, a state known as hypoglycaemia. It was discovered after World War 2 in 1942 and used widely thereafter to treat Type 2 diabetes by increasing a cell’s sensitivity to insulin. Ashcroft made the link between the similar role of ATP and Sulphonylureas on insulin release. In 1986, she tested it on individual potassium channels found in the insulin releasing cells. The drug was shown to bind to the potassium channel and cause it to close, triggering the release of available insulin from cells in the pancreas.
Ashcroft’s research also pointed towards the existence of a third type of diabetes: a type caused by a mutation in a single gene. Discovering the importance of potassium channels in insulin release, she believed that a certain type of diabetes was likely to be caused by a genetic mutation to the potassium channel. Yet to search for mutations, she first had to determine the protein structure of the potassium channel and find the DNA sequence which coded for it. It took her almost 10 years of arduous gene cloning to pinpoint the functionality of the channel protein.
By 1995, she had revealed the structure of what turned out to be a very complicated channel and by 1997, the function of each of its components were determined. By this time, Ashcroft knew the DNA sequence and could finally start screening patients for mutations. Ashcroft was convinced that a single gene mutation of the potassium channel must be present in newborns who had diabetes. These patients were diagnosed as diabetic at the unusually young age of around 6 months, which was never the case for the traditional Type 1 or Type 2 diabetes. It was wrongly assumed that, because no insulin was found being secreted, this was a rare form of Type 1 diabetes. Thus, the young patients were given insulin injections from birth: an intensely unpleasant experience for both them and their parents.
On the quest to find a mutation in human patients, Ashcroft collaborated with Professor Andrew Hattersley. In 2004, his lab tested and screened the blood from diabetic newborns and sure enough found just the mutation Ashcroft was looking for. About 50% of newborns with symptoms of diabetes had a mutation to the potassium channel protein, proving that the existence of neonatal diabetes is caused by a single genetic mutation. The mutation causes the channel to be insensitive to ATP and remain closed, preventing the release of insulin from otherwise functioning cells in the pancreas. This was a big eureka moment because there was already a well researched and readily available drug, Sulphonylureas, for related conditions.
 Susannah McLaren
Susannah McLarenAfter successful clinical trials in 2006, 90% of patients with neonatal diabetes have been transferred from insulin injections to the oral tablets of Sulphonylureas. The patients’ blood glucose levels were more stable with the tablets than they ever had been with insulin injections. The drug had a huge impact on the daily lives of many young children. They were no longer bound by strict dietary requirements or a rigid regime of insulin shots, all they needed was the tablets.
After this twenty-year odyssey, Frances Ashcroft’s endeavour to treat neonatal diabetes more effectively is still going strong. Questions remain for scientists to address: why do younger patients transfer more easily and successfully, and why does the required drug dose decrease with time? While neonatal diabetes is a rare condition, with only one in every 200,000 babies being diagnosed, it is debilitating for its sufferers. The treatment is an example of highly personalised medicine. The efforts of Ashcroft and other scientists have helped improve the quality of life of many children for years to come. Her ground-breaking, life-changing work has earned her the title of Dame Professor Frances Ashcroft, and she remains a true inspiration for a new generation of scientists.
